Patients with chronic conditions like Kidney Failure and so on often have many symptoms that bother them that are not necessarily directly related to their Kidney Disease. These symptoms are not clinically significant as they may not contribute to the risk of mortality or morbidity. They may not influence medical outcomes like other, more serious symptoms. Some examples are restless legs, constipation, sexual dysfunction etc. Symptoms like breathlessness, on the other hand, could be an indicator of different things like fluid overload or even a cardiac problem.
Some times, doctors might ignore symptoms that are not very serious. For the patient, however, these are bothersome and contribute to the overall burden of the disease. We think continuously about them and these, for us, could be more serious than some other symptoms which may cause more harm in the long run. Restless legs could bother us much more than itching, for example.
Palliative Care, which can help resolve many of these symptoms, needs to be incorporated into the treatment of all Chronic Kidney Disease (CKD) patients. The Oxford Dictionary defines Palliative Care as "relieving pain without dealing with the cause of the condition." Palliative Care is often confused as End-of-Life care or care that helps give the patient a death with dignity. Palliative Care is much broader. It can start very early in the life-cycle of the CKD patient. From Day 1.
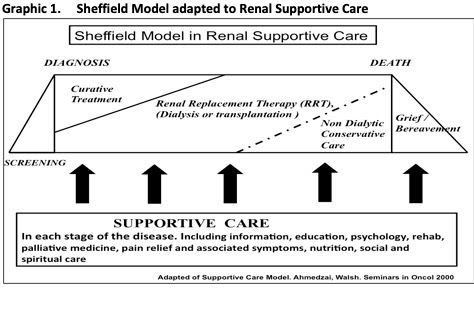
The above graphic shows very well, how Palliative Care or Supportive Care starts as soon as the diagnosis of CKD. Right through the initial attempts as curing it or putting the patient on some form of Renal Replacement Therapy (Dialysis or a Transplant) and after dialysis is stopped and the patient is put on Conservative Care, there is a role for Supportive Care.
A recent paper published in the prestigious journal, Nature, by Dr. Kam Kalantar-Zadeh talks about management of symptoms in CKD. The paper is open-access (thank you!) so feel free to take a look. They also have a fantastic table that lists all the commonly known symptoms that CKD patients face with some suggested interventions.
It is heartening to see the nephrologist community take our symptom-burden seriously and publish such manuscripts.
As patients, we need to have informed conversations with our doctors. We need to talk to them about our symptoms more clearly and request them to help with them. We should observe the nature of the symptoms, the frequency, any specific time of the day or on any specific days and so on. As much information as possible about the symptoms gives the doctors clues on what the reason is and how they can help us fix it. "Doctor, I have headaches" is much less helpful than "Doctor, I have headaches on the evenings of my non dialysis days which goes away by the morning"
So, let us all not shy away from talking about Palliative Care even when we are nowhere close to the end of our lives and incorporate it into our dialog. All of us will benefit from this.
Comments